Saturday, April 20, 2024
News and Views from the Global South
PAKISTAN: Unsung Heroines Bring Healthcare to Villages
Zofeen Ebrahim
- At eight in the morning 30-year-old Sultana Solangi steps out of her house ready for her day’s work. Wearing a black gown that shows only her eyes, she is shod in comfortable slippers and lugs a large black bag.
In her bag is an assortment of medical supplies: Paracetamol tablets and oral rehydration salts, bandages, condoms, contraceptive pills, iron and folic acid tablets, eye ointments, and antiseptic lotion.
Solangi, the sole breadwinner in her family of four, works as a lady health worker (LHW), employed by the government’s National Programme for Family Planning and Primary Health Care.
Launched in 1994, the programme now has a veritable army of 100,000 LHWs covering 60 percent of the population – the biggest outreach intervention in South Asia.
These women venture where few doctors dare to go, from congested cities to far-flung and underdeveloped rural areas, acting as the link between communities and the public health system.
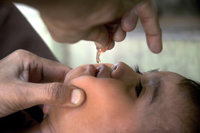
Over the years, their work has expanded to include health campaigns like administering polio drops to children under five, plus neonatal tetanus, measles, tuberculosis, and malaria control.
LHWs are particularly important in the rural areas where three-quarters of Pakistan’s population live, and where a trip to a health centre may require a hike of a couple of hours to as much as a day. Illiteracy is widespread in these areas and often customs prevent women from seeking health services without being chaperoned by a male family member.
Solangi cited the case of Zahida Sanghi, a woman Solangi’s age but already a mother of seven. Sanghi lives in People’s Colony, a community in Larkana city in Sindh province, some 322 kilometres from the southern port city of Karachi, which is part of Solangi’s coverage area.
“Zahida Sanghi was very weak and would not have survived another pregnancy. The husband is jobless. It took close to two months to convince her mother-in-law that it was all right for her to get a tubal ligation done since her family was complete. This is all part of my job,” she said.
Every day, Solangi and her colleagues cover between five to 10 houses and talk to women like Sanghi about the importance of antenatal check-ups, vaccinations, safe delivery, the use and making of oral rehydration salts, and modern methods of family planning.
They also hold about eight group sessions each month where they discuss with local women issues related to mother and child health.
Yet despite the LHW programme, Pakistan remains a maternal and infant health hotspot.
The Pakistan Demographic and Health Survey (PDHS), conducted from 2006 to 2007, shows an infant mortality rate of 78 deaths per 1,000 live births. It also shows a mortality rate of children under five years old of 94 deaths per 1,000 live births. This means one in every 11 children born in Pakistan dies before reaching his or her fifth birthday.
The maternal mortality rate of 276 per 100,000 live births is also far too high, and has remained virtually unchanged since 1991.
Sadiqa Jaffery, president of the National Committee on Maternal and Neonatal Health, said the statistics would be much worse without the LHWs on the ground.
“It’s been established that where LHWs are present family planning services and routine immunisation is better. The problem is that the coverage is not blanket,” Jaffery said.
But Farid Midhet, founder of the Safe Motherhood Pakistan Alliance, remains unconvinced of the impact of LHWs. “Family planning is the cornerstone of women’s health services and it still eludes millions,” he said.
Midhet cites the 2007 PDHS, which says less than a third of married women use family planning methods – only 14 percent use a modern temporary method, and less than five percent receive their contraceptives from the LHWs. “The reason is that many LHWs are only there on paper and rarely make visits or provide services,” he said.
Midhet said a more efficient way of reducing maternal mortality would be to bring primary healthcare clinics closer to women, providing easy access to emergency obstetric care through secondary hospitals, and providing affordable ambulance services which could be called using mobile phones.
As for reducing infant mortality, Midhet suggests improving mothers’ education, promoting family planning, and making well-baby care available and accessible to all, among other interventions.
He also proposed providing prompt and effective treatment for diarrhoea and respiratory infections among infants. “These services are of extremely poor quality in public hospitals and people resort to the private sector, which is dominated by quacks and is completely unregulated,” Midhet said.
But Asif Aslam of the U.N. Children’s Fund (UNICEF) pointed out that, “few doctors and paramedics are willing to serve in facilities in the remote villages, and less than 26 percent of people from the community venture to the government-run health centres.”
Jaffery said despite their work, LHWs still do not enjoy their rightful status in the community. “Their appreciation in the community is just not there, salaries are not paid on time, if paid at all,” she said.
Solangi said it took her over five years to get accepted in People’s Colony. “Our work holds no value for the community. It takes much perseverance and cajoling to get into homes.”

 Print
Print