Friday, April 17, 2026
News and Views from the Global South
MALAWI: Fears of Sustainability of New ART Regime
Charles Mpaka
- As government prepares to roll out the expensive new antiretroviral treatment regime recommended by the World Health Organisation (WHO) this month, there are fears about the programme’s sustainability after two recent proposals for funding were rejected by the Global Fund.
But the new regime costs almost five times as much as the current one. Principal Secretary for HIV/AIDS and Nutrition in the office of president and cabinet, Mary Shawa, says government currently spends about 34 million dollars annually on ARVs. The new regime will cost up to 105 million dollars a year.
But she insists that despite the fact that the Global Fund has rejected two proposals from Malawi worth a total of 564 million dollars, government will go ahead using its own resources to meet the cost of the new treatment regime. “The president has directed that we migrate to the new regime,” she says.
But the Global Fund, United Nations and Department for International Development (Dfid) support 80 percent of Malawi’s health budget.
Reasons for the rejection have varied. Some say it was due to government’s failure to include in its proposal minority groups, such as same sex relationships, which are illegal in Malawi. Shawa says, however, that government included gays and lesbians in its proposal.
She described the rejection as normal and said government would find a way of ensuring that patients access the new treatment this year.
But the shortage of aid is not just from the Global Fund. The British government announced in May it is suspending all new aid to Malawi following the expulsion of the British envoy for accusing President Bingu wa Mutharika for being autocratic. Germany is also withholding part of its aid for alleged human rights violations by government. This has led to fears that Malawi will not manage the new regime.
But government has announced it is migrating to the new regime regardless and will be able to fund the programme for the next four and half years using its own resources. According to a study commissioned by government on how to implement the new ART guidelines, government will now have to provide treatment to more people. The study found that adopting the new procedures would entail that people living with HIV/AIDS would have to start taking drugs at a higher CD4 count of 350. This would raise the total number of patients on ART by 50 percent. Currently, there are 250,000 people receiving free treatment in public hospitals in Malawi, government records say.
Asked where exactly government would get the money from other than the Global Fund, Shawa said the money will come from other sources including domestic ones. But an inside official at the National Aids Commission says government is preparing another proposal to the Global Fund for the next round.
“I wouldn’t lie that government can manage it all alone for too long. For now though, the two rejections (by the Global Fund) helped government to look elsewhere for money, hence the current position that we can still support the programme for some time. If anything, absence of donor money means resources would have to be taken from other sectors. But we are confident we won’t go in that direction,” said the source.
Health activists are unsure whether government can sustain the new programme without Global Fund support but they applauded government for migrating to the new regime.
Martha Kwataine, the executive director for Malawi Health Equity Network (MHEN), a grouping of non- governmental organisations in health, says it is the constitutional mandate of government to provide quality health care services to its citizens regardless of how much it costs.
“The cost (of running the new regime) is very high but quality has a price. The lower the price, the lower the quality, and consequently the negative side effects of the drugs. The cost is worth it because there is no price tag for life. Considering the negative side effects that people living with HIV have had, especially women, it is time for Malawi to change to the new regime,” she said.
And there are some who cannot wait for the new regime. While waiting in a queue to get her antiretrovirals at Chiradzulu District Hospital just outside Blantyre, a female patient showed IPS her legs claiming they were disfigured because of her ART.
“Honestly, the only good thing with these drugs is that I am still alive. But the side effects make me very uncomfortable. My legs were not like this. When I started taking the drugs in 2008, I felt pain in the legs for about four weeks. Doctors just said it was the side effects of the treatment,” she said, opting for anonymity.
Two other women on the queue complained about experiencing nausea and stomach protrusion.
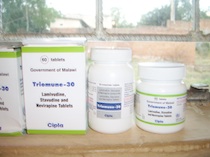
The last time Malawi reviewed its AIDS treatment protocol was in 2008 when it adopted the current first-line combination of stavudine, lamivudine and nevirapine.

 Print
Print