Monday, June 1, 2026
News and Views from the Global South
HEALTH-ZIMBABWE: Government Promises to Rebuild Health System
Stanley Kwenda interviews HENRY MADZORERA, minister of Health and Child Welfare
- The resuscitation of Zimbabwe’s health care system has been identified as one of the major challenges facing the country by the country’s new unity government.
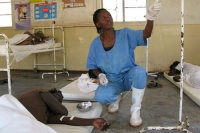
Caring for a cholera patient: the health system faces massive challenges with almost no budget. Credit: Paul Garwood/WHO
A major referral hospital, Harare Central Hospital, which had been closed since November 2008 due to lack of equipment, drugs and health workers, has recently been re-opened but is far from being fully operational.
Zimbabwe’s health minister, Henry Madzorera, will have to solve a wide range of problems to get the country’s public health system back on track, such as water shortages, malfunctioning equipment, a de-motivated workforce and a general lack of finances.
IPS: You have become health minister at a time when the country faces a devastating cholera epidemic. What immediate measures have you put into place in response? Henry Madzorera: Cholera continues to be a source of sickness and death in many towns and villages. A reasonable response was mounted a few months ago when the donor community was asked to come in and help. Many agents, like UNICEF, Médecins Sans Frontières, Red Cross and church organisations, to name but a few, helped with much needed supplies and human resources to fight cholera.
A fund was established to support health care workers, not just at the cholera camps, but throughout the country. This general strengthening of our health care centres is an integral part of the war against cholera. From the ministry of health’s perspective, we are doing fine on the curative side. Case fatality rates have dropped to under one percent and that’s acceptable by global standards.
Please note that water and sewerage failures are the cause of this sustained onslaught on our people. We are working hard to encourage local government to deal with the problem.
Prevention is the only answer to cut cholera. We have educational campaigns going on, such as television and radio ads and posters, but without ready access to clean water and sanitation, this education is of limited value. Zimbabweans must start learning how to demand what is rightfully theirs.
IPS: The national health system has virtually collapsed. How will you start rebuilding it? HM: We are negotiating with various partners such as UNICEF, World Bank and others, for infrastructure rehabilitation, repair of equipment and transport, supply of drugs, etc. As the ministry of health, we will continue with our educational campaigns to improve household hygiene and implement a coordinated health plan once funds are available.
IPS: Rebuilding the public health sector will require significant amounts of money, yet the new government is inheriting a bankrupt system. What budget has been allocated to fix this? HM: You correctly point out that there is no money in the ministry. There is no formula for funding health care at the moment. That’s why we are relying on our international partners for funding until Zimbabwe is back on its feet economically.
Medical taxes have been contributing a negligible amount to health care financing in Zimbabwe. We plan to eliminate these in the long term, but first we must come up with innovative ways of funding health care. This we can only do with the involvement of all our communities, including the patients, the private sector, government and the donor community.
IPS: The plight of health workers who have been on strike for many months is ongoing. How will you address health workers’ demands for higher salaries? HM: We now have the health sector support fund [since Nov. 2008], which is paying out allowances to health workers of $100 a month to as a retention incentive. As a result, 95 percent of our workers are back to work. Obviously they hope the once-off allowances will continue.
IPS: What is your strategy to rehabilitate rural health facilities, some of which have been closed down? HM: Its work in progress. We are working with [international] partners to first make sure that rural facilities have the personnel, drugs and equipment and then move on to other issues, such as upgrading facilities. We are taking over a collapsed system.
IPS: HIV and AIDS remain a big problem in Zimbabwe with a HIV prevalence rate of 15.3 percent. This is exacerbated by poverty and lack of access to health care. How will you ensure HIV treatment and care? HM: We have grants from the Global Fund to Fight AIDS, TB and Malaria. $496 million were approved in round eight of the Global Fund. We are also trying to ensure that the flow of funds [from government to health facilities] improves. If all processes go well, we should be able to access some of these funds by Jul. 2009. There is great potential for achieving universal access to [antiretroviral] treatment soon.

 Print
Print



