Saturday, April 20, 2024
News and Views from the Global South
NAMIBIA: Investing in the Health of Farm Workers
Servaas van den Bosch
- In one of the most sparsely populated countries on the planet, people travel up to 200 kilometres in the simmering heat to see a nurse or get basic medication.
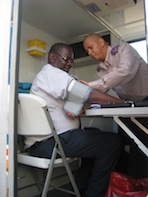
Registered nurse George du Plessis takes a patient's blood pressure in the mobile clinic. Credit: Servaas van den Bosch/IPS
Most people who fall ill on a Namibian farm wait out their illness. They rather risk developing a chronic condition than making the arduous trip to a far away clinic in the forty degree Celsius heat. And even if they go, they most likely will have to wait for a long time before a medical officer sees them. In addition, the chances of them being sent home with an over-the-counter painkiller is high.
To fill this gap in primary healthcare provision Dutch non-governmental organisation PharmAccess, together with the health ministry and the private sector have started a mobile clinic in one of the most remote regions of Namibia, in rural Otjozondjupa.
The project called Mister Sister has converted trucks into mobile clinics, receives medicine, vaccines and consumables from the health ministry, and funding from a growing complement of corporate sponsors.
“Mister Sister addresses an extremely important and often not recognised problem,” remarked professor Rich Feeley from Boston University and advisor to the project at the project’s launch in mid-June. “Even when the costs are free, getting to the healthcare facilities is a problem.”
In June the first Mister Sister mobile clinic commenced its month-long route along farms in the rural Otjozondjupa Region some 100 kilometres (km) from the capital Windhoek. Ultimately the service will operate three mobile clinics with a budget of 230,000 dollars each per year.
The average distance to a clinic in Namibia is 69km, to a doctor 99km, hospitals are approximately 107km away and for a dentist one travels 170km. But these are averages. In a country roughly the size of Pakistan, but with only two million inhabitants, having to travel 200km to access healthcare is no exception.
Though classified as an upper middle-income country by the World Bank, Namibia has the world’s highest income inequality on record and only 15 percent of its people have medical health insurance.
“Private insurers will only service the insured. We wanted to put in place a system that delivered unified care. Farm workers and their dependants have free access to our healthcare, while for teachers or police officers at roadblocks we can claim the treatment from their insurance companies,” said Ingrid de Beer, Namibian general manager of PharmAccess in Namibia.
She adds that the system is unique in the way it brings public and private players together. De Beer: “It doesn’t make sense to have a private and a public system servicing the same population. Instead PharmAccess runs the service, with contributions in kind from the government and monetary input from the employers.”
“We in the private sector have a habit of criticising a (health) system that doesn’t work,” commented Derek Wright, president of the Agricultural Employers Union, which promotes the initiative among its members. “But in the agricultural sector we have learnt that it is better to find a solution. It’s important to invest in the health of our employees and their dependants.”
While the clinics are free for workers, farmers along the route have to pay a 700-dollar annual participation fee, regardless of the size of the staff complement or its dependents. So far 27 commercial farmers have signed up.
Sakkie Coetzee, chief executive officer of the Namibia Agricultural Union thinks it is a good deal for the farmers.
“There are a lot of advantages. The clinics save the farmer time and will undoubtedly increase productivity on the farms. It makes sense for farmers to pay the contribution. By taking healthcare provision in their own hands they will save money in the end.”
Another benefit of the public-private partnership is that red tape is reduced to a minimum, said Feeley.
“In this setup its easier to replace a starter motor, without first having to obtain three quotes. Or when the blood pressure pump breaks, the supply lines are probably infinitely shorter.”
“It is also an unique opportunity to put in place evidence-based management, learning from the project as we go along and implementing these lessons here and elsewhere,” he added.
“It’s a very good initiative because access to healthcare in these areas is a big, big challenge for the rural population, especially farm workers. We give them good treatment, the best actually,” George du Plessis, who heads the mobile clinic’s team, told IPS.
The teams consist of a registered nurse, an enrolled nurse and a driver. Du Plessis and his colleague see about thirty patients every day.
“Many patients suffer from neglected chronic conditions such as diabetes and high blood pressure,” he explained. “With an elevated blood pressure it is easy to get a stroke, yet the condition can be treated easily and on our next visit we simply bring three months worth of drugs so that the patient doesn’t have to go to hospital to renew the prescription.”
De Beer estimates that such ‘medical backlogs’ constitute a part of the clinic’s early work. But by enrolling these patients on an automated system, listing their conditions and starting treatment later cost to the healthcare system and the agricultural sector can be avoided.
“Other conditions that we encounter are back pains and headaches from working in the fields all day long in the burning sun and respiratory problems in kids, such as coughing and sneezing,” continued Du Plessis, whose lapel insignia identifies him as an experienced nurse, qualified in delivering babies, treating psychiatric patients and offering community health care.
“Many children also are behind with their immunisations, which is a big problem. The initial vaccinations at birth in the hospital are not followed up because of the long distances.”
Du Plessis says the clinic also plays an important role in voluntary HIV/AIDS counselling, as well as family planning. “Sometimes a single mother has six kids and can hardly cope. Employers, therefore, encourage women workers to make use of family planning to prevent unwanted pregnancies.”
It’s a far cry from the days when government officials handed out condoms and Panadol on their visits to rural areas.
“We sit down with the patients and take as much as thirty minutes to talk about their problems. The farm workers respect you for that. They really appreciate the service,” Du Plessis said.

 Print
Print



