Thursday, May 28, 2026
News and Views from the Global South
Countdown to ZERO
Nigeria Wakes Up to its AIDS Threat

Nigeria accounts for one third of all new infections among children in the 20 worst hit countries in sub-Saharan Africa. Credit: Sam Olukoya/IPS
- Tope Tayo’s marriage broke up 11 years ago after she tested positive for HIV. Her angry and embarrassed husband took away their only child. Three months later, when the one year old boy tested positive, the husband dumped him with Tayo and absconded.
“He abandoned us as if we had committed a crime but I told him HIV is not a crime,” Tayo told IPS.
She was jobless and the husband paid no maintenance. “I walked the streets crying, I was living on charity,” Tayo recalls.
The runaway man who abandons his HIV positive wife and children is a common feature in Nigeria, says Rosemary Hua, coordinator of the First Step Action for Children, an organisation that advocates for child rights.
“Fathers withdraw their support because they feel there is no need to invest in a child that is likely to die young,” Hua told IPS.
Nigeria’s HIV infection rate of 3.2 percent appears low in comparison to southern Africa’s, but with a population of 173 million, it translates into huge numbers – 3.4 million Nigerians lived with HIV in 2013.
Of these, 430,000 are children under 14, according to a recent report of the Joint United Nations Programme on HIV/AIDS (UNAIDS). Nigeria accounts for one third of all new infections among children in the 20 worst hit countries in sub-Saharan Africa.
173 million population
3.2 % HIV prevalence
3.4 million Nigerians live with HIV
51,000 new child infections
220,000 new infections among all ages
190,000 HIV positive pregnant women
52,500 HIV positive pregnant women receive ARVs
70% of HIV positive pregnant women do not receive ARVs
47, 300 children on ARVs, or 12% of all infected children
593,000 people on ARVs, or 21% of all infected people
210,000 AIDS-related deaths
Little decline in deaths between 2005-2013
Source: UNAIDS 2014
The report says Nigeria faces “the triple threat of high HIV burden, low treatment coverage and no or little decline in new HIV infections.”
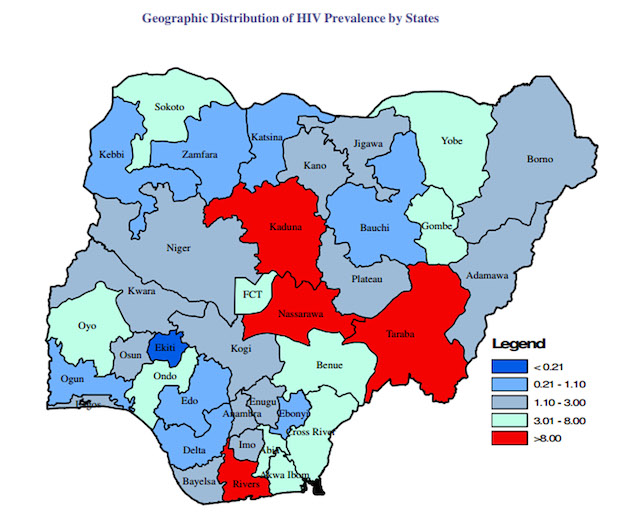
Moreover, the national HIV rate conceals sharp disparities among the 36 states: in four, prevalence ranges from eight to 15 percent.
Why women avoid testing
Tayo and her son have been taking antiretroviral drugs for the last 11 years. They are lucky. Fewer than 600,000 Nigerians are on treatment, or 20 percent of those who need it.
Low treatment coverage perpetuates misconceptions and stigma, as Tayo’s story show.
Abandonment usually translates into economic hardship. Half of women are unemployed in Nigeria.
“The desperation to take care of herself and her child could drive an HIV positive woman into sexual activities to raise money and this could further spread HIV,” says Lucy Attah, a gender activist who lives with HIV. She is executive director of Women and Children of Hope Foundation, which helps HIV positive women, and where IPS met Tayo.
Tayo told IPS she avoided testing for HIV while pregnant. Nigerian public hospitals do routine HIV testing of pregnant women but fear of discrimination if found positive led Tayo to a private hospital where testing was not required.
“It is the biggest regret of my life,” she told IPS.
One reason that pregnant women shun testing, says Hua, is health workers’ “lack of professionalism by not keeping HIV results confidential.”
“At times we had to transfer patients to other hospitals far from where they live because of the disclosure of their HIV status,” she told IPS.
Some health workers avoid any contact with HIV positive women because they mistakenly believe they can contract the virus by mere touching, says Attah.
“On the surface, it seems there is a lot of awareness among health workers but in reality there is a lot of stigma,” says Attah.
An anti-discrimination and confidentiality law has been approved by both houses and is waiting for President Goodluck Jonathan to sign it.
But Nigeria needs more than laws to address the epidemic.
In 2012, UNAIDS described the country’s response as “stagnant” and requiring “a massive effort.”
Nigeria accounts for 13 percent of all HIV positive people and 19 percent of all AIDS-related deaths in sub-Saharan Africa, according to UNAIDS.
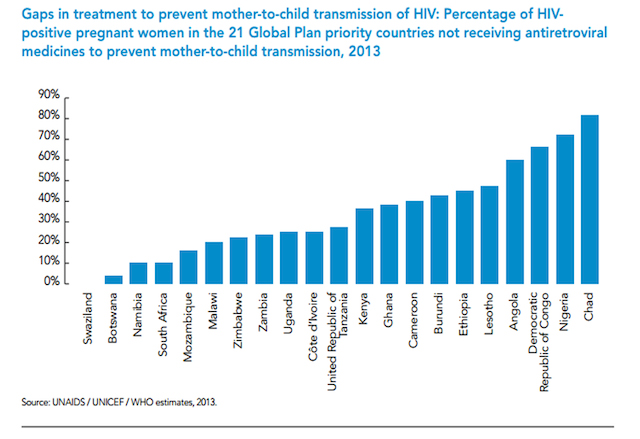
Only Chad ranks lower than Nigeria in treatment coverage of HIV positive pregnant women. (see graph)
Some good news
Since that damning description, the government has taken bold steps to reduce transmission from mothers to babies (PMTCT) among the 12-worst hit states.
PMTCT coverage went up to by 27 percent in 2013, a significant increase from 19 percent in 2012, according to the United Nations Children’s Fund (UNICEF).
Some states doubled or tripled the number of clinics providing HIV services, bringing the number of PMTCT sites to 2,216 – still far from the 16,400 required for adequate coverage.
The annual number of new child infections went down from 60,000 in 2012 to 51,000 in 2013.
But, with two in three pregnant women shunning antenatal care, the challenge will be reaching them through improvement of services and outreach.
“We must go to them instead of waiting for them to come to the health facility,” Arjan de Wagt, chief for children and HIV with UNICEF in Nigeria, told IPS. “Otherwise, children will continue dying of AIDS unnecessarily.”
Edited by: Mercedes Sayagues

 Print
Print