Languages
Friday, April 24, 2026
News and Views from the Global South
Bitter Pill: Obstacles to Affordable Medicine

EAST AFRICA: ‘It’s Not a Heartless Mother Leaving a Child Behind, Just One Who Wants to Survive’
On the road between the Kenyan and Somali border lie the dead bodies of children who have succumbed to the famine and the hardships of making the journey from their drought-stricken villages to Kenya.SWAZILAND: Economic Crisis Means Short Supply of ARVs
Swaziland’s economic crisis has affected its ability to provide healthcare as the country’s buffer stock of antiretrovirals (ARVs) has fallen below the prescribed three-month supply.KENYA: Providing ARVs to HIV-Negative People Will Strain Resources
When Lucy Omollo found out that her husband was HIV-positive six years ago, the couple thought the best way to prevent her from becoming infected with the virus was not to have sex.HEALTH-UGANDA: Self Medication Blamed for Increased Drug Resistance
In pharmacies in the heart of Kampala men and women line up to buy drugs that you usually need a prescription for, like Coartem, a drug used to treat malaria.
UGANDA: In Search of Better Medical Care
Even though government health services are free, Grace Nafungo Kutosi doesn’t mind paying the two thousand shillings (about one dollar) when she visits the non-governmental Beatrice Tierney Clinic in Bumwalukani village. In fact, paying the fee at the clinic, which is a 20-minute walk from her home, is cheaper than her having to travel to the nearest government clinic almost seven kilometres away.
KENYA: Strategy to Counter Counterfeit Medicine
In Kenya buying medicine from any unregistered pharmacy outlet means that you are running a higher risk of buying either substandard or counterfeit drugs that form 30 percent of all drugs sold in the country.“BRICS Can Ensure Affordable Drugs”
While ‘data exclusivity’ clauses will not feature in the India-European Union free trade agreement (FTA), the threat posed by the impending deal to the world’s supply of cheap generic drugs is far from over.
KENYA: People Dying Because of Lack of Anaesthetics
One person dies weekly in Kenya due to a shortage of anaesthetics and the situation is worse in slums and rural areas across the country.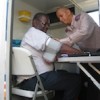
NAMIBIA: Investing in the Health of Farm Workers
In one of the most sparsely populated countries on the planet, people travel up to 200 kilometres in the simmering heat to see a nurse or get basic medication.
UGANDA-HEALTH: When Women Go Without Needed Contraceptives
When the monthly contraceptive injection that Bernadette Asiimwe, a mother of four, got from government health centres in western Uganda was out of stock for weeks, she fell pregnant with her fifth child.
KENYA: No Longer Forced to Buy Ineffective Anti-Malarial Drugs
People in Western Kenya are now able to buy effective anti-malarial drugs at low prices thanks to the success of the Global Fund’s subsidy programme, and thanks to honest pharmacists who are reselling the drugs at the recommended low prices.UGANDA: Distribution Policy Means Not Enough Drugs for Clinics
The nurse at Najembe Health Centre in Buikwe district says the centre’s supply of malaria drugs will be finished in two days. A malaria epidemic has hit the area and the demand for the drugs is high. But the centre, which serves the entire sub-county, will have to wait up to six weeks before their supply will be replenished.Another Push for Reproductive Rights
By 2015, women demanding family planning products and services in the developing world will likely reach 933 million, a terrific increase from the current 818 million women demanding access to these basic reproductive commodities.
HEALTH: High Drug Prices Hamper Drug-Resistant TB Treatment
Access to treatment for drug-resistant tuberculosis (DR-TB) remains compromised, especially in developing countries, because too few pharmaceutical companies manufacture quality-assured drugs. Lack of competition has led to skyrocketing prices and this means that public health budgets are quickly spent.
SIERRA LEONE: Substandard and Counterfeit Drugs Flood the Market
Bubble-wrapped pills are scattered across the crude table in a busy market beside crumpled boxes of lubricant, paracetamol and anti-fungal powder.Mental Health Work in Humanitarian Crises
When the devastating ‘Boxing Day' tsunami hit Sri Lanka in December 2004, claiming over 35,000 lives and rendering 1.5 million people homeless, the World Health Organization (WHO) was confronted by a second disaster soon after it arrived to begin relief efforts in early January.
SIERRA LEONE: A Quarter of Vital Donated Drugs Missing or Stolen
Three-year-old David bolts up from his feverish stooper as a needle pricks his thumb, producing a tiny bead of blood. He looks down horrified but is too exhausted to cry and falls back into his mother's lap as the blood is wiped awayAfrica Becoming More Attractive to Indian and Other Investors
A reduction in red tape and an improvement in political conditions means that sub-Saharan Africa is becoming a more attractive destination for foreign direct investment, especially from India.IBSA: Pro-Western Mindset Hinders India-Brazil Pharma Deals
Cooperation between India and Brazil in pharmaceuticals and medical biotechnology has begun to falter, because Indian authorities would rather collaborate with western counterparts than those in developing countries, new research shows.UGANDA: The Value of Immunisation Programmes
GAVI, the Global Alliance for Vaccinations and Immunisation, secured pledges of 4.3 billion dollars from donors in London on Jun. 13 with the aim of securing funding to ensure life-saving vaccinations for every child on the planet.
MALAWI: Fears of Sustainability of New ART Regime
As government prepares to roll out the expensive new antiretroviral treatment regime recommended by the World Health Organisation (WHO) this month, there are fears about the programme’s sustainability after two recent proposals for funding were rejected by the Global Fund.« Previous Page — Next Page »










